Physical therapy is recognized for its essential role in aiding patients on their way back to mobility, strength, and independence. Recent developments at Utah State University (USU) and within Federal parameters have cemented physical therapy’s significance and highlighted areas needing change within its practice.
Utah State University has opened a physical therapy clinic as part of the Sorenson Legacy Foundation Center for Clinical Excellence, which offers a plethora of services including manual therapy, therapeutic exercise, and the unique therapeutic feature of aquatic therapy.
For northern Utah residents, this state-of-the-art facility introduces a method to treat physical aches, reduce pain and regain functional mobility. The USU clinic is led by experienced professional, Megan Bressel, who brings new and improved physical therapy methods to the Center.
One intriguing development is the Hydroworx pool’s introduction, which allows for aquatic physical therapy. The pool’s benefits include its adjustability which gives those who are mobility-challenged the ability to enter the water safely. It also features jets to provide resistance training and an underwater treadmill that can be adjusted for varying speeds. Given that aquatic therapy can offer resistance, buoyancy, and hydrostatic pressure benefits, Bressel insists that it can provide an accelerant to the healing process.
However, these advancements in physical therapy are counterbalanced by the hurdles faced by some practitioners when serving Medicare beneficiaries. Dr. Sean Wells, who operates a mobile physical therapy practice in Northern Florida, has been forced to refrain from treating many patients due to their Medicare status.
Dr. Wells established his business in 2011 as one of Florida’s first cash-based physical therapy initiatives, a model that allows both patients and providers to bypass the limitations and paperwork of insurance systems. Despite this, physical therapists are not listed among professionals who have the legal right to opt out of Medicare and establish private contracts with Medicare beneficiaries.
The law’s bureaucratic technicality, which sees physical therapists classified neither as “physician” nor “practitioner,” poses a significant hindrance to patient care. Prevented from treating Medicare patients, physical therapists face potential severe penalties and professional alienation. This rule means physical therapists must halt treatment in times of patient health crises.
To combat this issue, Dr. Scott Gardner formed the United Physical Therapy Association (UPTA) in 2024. UPTA advocates policies that widen healthcare accessibility and empower providers to offer cash-based services to Medicare patients.
With backing from Pacific Legal Foundation, Dr. Wells and UPTA have launched a federal lawsuit aiming to challenge Medicare’s discriminatory ban on physical therapy services undertaken through private-pay. Dr. Wells maintains that patients ought to choose their provider and that professionals should be free to perform their duties without fear of government backlash. The lawsuit emphasizes the constitutional right to equal treatment and the capability to earn a living, free from arbitrary government interference.
The recent developments within physical therapy underline its evolving status within the healthcare arena. Despite regulatory hurdles and bureaucratic issues, the emphasis remains on providing accessible, flexible, and efficient facilities and treatment to patients, furthering its presence as a fundamental part of healthcare provision.
Physical therapy services are making headway into mainstream healthcare, with a variety of treatments now available and increasingly accessible. Physical therapy, a vital part of the rehabilitation process, is now being offered by Sanford Health West Fargo, where patients can work one-on-one with experienced therapists.
According to Sanford Health lead physical therapist, David Tompkins, physical therapy is crucial to patients’ recovery and return to their normal lives. Sanford provides a range of specialized services and therapies, including dizziness treatment, dry needling, LSVT BIG treatment for Parkinson’s, lymphedema therapy, orthopedic care, pain management, postoperative services, stroke rehabilitation, and women’s health care services.
Sanford West Fargo offers physical therapy Monday to Friday, aiming to be a convenient choice for residents seeking high-quality treatment. However, for those unable to physically access therapy centers, global patients now have a newfound access to physiotherapy through online services such as Vyana Care.
Virtual physiotherapy has now become a viable solution in overcoming geographical distance barriers, replacing frustrating waiting times and extended drives with immediate access to professional care. Vyana Care has expanded its online offerings to cater to patients worldwide. This aligns with the paradigm shift in healthcare, whereby high-quality care is not dependent solely on proximity to physical locations.
The World Health Organisation estimates that approximately 1.71 billion people suffer from musculoskeletal issues, representing the leading cause of global disability. Back pain is the most common cause, affecting nearly 619 million people – a figure projected to rise to 843 million by 2050.
However, access to high-quality physiotherapy is inequitable, with waiting time, cost, and lack of trained personnel preventing patients from receiving the necessary treatment. Vyana Care seeks to address this disparity by providing personalized online physiotherapy to patients across the globe.
Contrary to the perception that online physiotherapy equates to simple YouTube exercises, virtual physiotherapy is a structured and clinically-led process that mirrors in-person clinic procedures. It begins with a certified physiotherapist conducting a comprehensive examination via video consultation, followed by the design of a customized rehabilitation program. The patient undergoes specific exercises with regular follow-ups to monitor and adjust the regimen.
A wide range of physiotherapy treatments is available through virtual care, including chronic neck and back discomfort, shoulder injuries, knee pain, stability and mobility problems, cervical spine issues, postural corrections, neurological rehabilitation, sports injuries, and more.
Global access to virtual care represents a significant step in democratizing healthcare. It ensures that geographical location, financial constraints, or any other barriers do not hinder patients from receiving quality clinical care. Platforms like Vyana Care are pivotal in this transformation, where patients worldwide can get top-quality, personalized care previously only available to those in specific regions or income brackets.
The physical therapy sector continues to expand and innovate, offering increasingly customized and efficient treatments for a range of conditions. One significant development recently was the opening of a new JAG Physical Therapy practice in Cranford. This is the eighth JAG location in Union County and it offers comprehensive physical therapy treatment, concussion rehabilitation, sports medicine, and at-home program services. The company focuses on creating personalized treatment plans for patients suffering from general orthopedic, sports and soft tissue injuries.
The global medical rehabilitation services sector is projected to grow significantly, driven by demographic shifts and the rising prevalence of chronic diseases. By 2034, the market is expected to be worth around US$ 454.1 Billion, expanding from US$ 246.5 Billion in 2024 at an annual growth of 6.3%. North America currently dominates the market, accounting for over 45.9% of the global share in 2024.
Physical therapy held the leading position in the therapy segment in 2024, due to the high demand for musculoskeletal rehabilitation and post-surgical recovery programs. The orthopedic section was predominant in the application segment, followed by the cardiologic section, which is expected to grow due to the increasing burden of cardiovascular diseases.
However, the sector faces some significant challenges. U.S. tariffs have increased the cost of essential medical equipment, causing some disruptions in the medical services supply chain which can affect patient outcomes. Also, financial barriers and insurance limitations impose restrictions on patient access to rehabilitation services, particularly in low- and middle-income countries.
Despite these challenges, there are opportunities for growth. Tele-rehabilitation and digital health platforms are gaining traction as they facilitate the remote delivery of physical therapy services. Also, the integration of advanced technologies like AI, robotics, and wearables into rehabilitation therapies continues to drive the evolution of the industry.
Moving forward, the expansion of tele-rehabilitation and wearable technology offers significant opportunities for the sector, enabling therapists to reach more patients and deliver personalized and efficient care remotely. With the continued support of global initiatives to strengthen rehabilitation services and the expanding adoption of advanced technologies, the physical and occupational therapy sectors are set for significant growth in the coming years. This expansion will provide enhanced and more accessible services for patients globally, helping to improve functional outcomes and the quality of life for many.
“State of Direct Access to Physical Therapist Services” to use this comprehensive resource to better understand the opportunities and challenges of driving unrestricted access to physical therapy services.
3. Iowa City’s Innovative Physical Therapy offers virtual appointments amid pandemic
Iowa City’s Innovative Physical Therapy has adjusted to the challenges brought about by the pandemic, offering virtual appointments to patients who need the services but cannot leave their homes. This innovative move uses telehealth to provide physical therapy services, including picking up on physical cues via a video chat to guide patients through their exercise routines.
Clinic Director Jake T. Powell shares that so far, the online consultations have been successful and greatly appreciated by patients, especially the elderly and those with mobility issues. The platform is used to discuss treatment plans, instruct patients on specific exercises, and allow patients to ask questions directly to the therapists, all in the safety of their home environment.
However, Powell also mentions that they still offer in-person services for those who prefer them, maintaining a safe and sanitary environment by closely adhering to COVID-19 guidelines set by public health officials. The combination of virtual and in-person sessions allows flexibility for their clients and ensures accessibility of services.
4. MobilityFit Physical Therapy Adds New Pain Management Services
MobilityFit Physical Therapy in Cincinnati, Ohio, has expanded its service offerings by adding new pain management therapeutic services to its existing catalogue. The move is geared towards catering to an increasing number of patients suffering from chronic pain, a widespread issue exacerbated in part by the ongoing pandemic, causing people to be less active and sit for longer periods.
Added services include neural mobilization, a gentle technique aimed at relaxing the nervous system; myofascial release, a therapy that involves applying gentle, sustained pressure into the myofascial connective tissue layers; and manual lymphatic drainage, a type of massage that encourages the natural drainage of the lymph from the body tissues.
The therapists at MobilityFit Physical Therapy are also trained in cognitive behavioral therapy techniques to help patients manage their pain more effectively. The clinic strives to take a holistic approach to pain management, integrating physical treatments with psychological interventions to achieve the best possible outcome for their patients.
5. Trends in Physical Therapy: Emphasis on Wellness and Preventive Care
Physical therapists are increasingly focusing on wellness and preventive care, in contrast to the traditional reactive model of healthcare. Therapists are offering sessions focused on improving mobility, strength, and balance, all aimed at reducing the risk of injuries and health issues down the line.
Furthermore, physical therapists are utilizing equipment such as wearable technology to monitor patients’ movement and provide feedback on their performance. This innovative technology allows therapists to measure progress effectively and make personalized adjustments to each patient’s treatment plan.
In a bid to combat the rise of sedentary behavior and poor posture due to the increase in remote work, therapists are also introducing office ergonomics programs, conducting assessments, and providing recommendations for arrangement and use of workspaces, helping to minimize physical strain and prevent work-related musculoskeletal disorders.
6. Physical Therapy Research Highlights: The Power of Exercise for Mental Health
A research study published in the Journal of Physical Therapy Science revealed that regular exercise can improve mental health conditions such as depression and anxiety. The study looked at 123 participants, aged 60 and above, and found that those who engaged in a regular physical therapy regimen reported a significant improvement in their mental wellbeing.
Planned and supervised by trained physical therapists, the exercises focused on increasing strength, improving balance, and promoting mobility – all of which contribute to not just physical wellbeing but also mental health. The study underscores the role of physical therapy in the spectrum of healthcare services, reiterating that it doesn’t only treat physical ailments but also contributes significantly to mental health rehabilitation.
7. Future Prospects: AI and Robotics in Physical Therapy
While the human touch, understanding, and empathy play crucial roles in physical therapy, the field isn’t immune to the ongoing technological revolution. Developments in AI and robotics might change the way therapists conduct their practice in the future.
Already, robotic device-assisted therapies for stroke patients have seen promising results, helping them regain motor functions more efficiently. AI, in tandem with wearable devices, can provide valuable data and predictive analytics to help therapists design personalized treatment plans.
While AI and robots will never fully replace human therapists, they can serve as invaluable tools that aid in the goal of providing patients the best possible care. Combining technological advancements with human expertise will enable therapists to deliver physical therapy services that are effective, personalized, and cater to a broad range of patient needs.
Investing in physical therapy is an investment in overall health, offering individuals a chance to live their lives fully and actively, regardless of their age or physical conditions. Whether to recover from an injury, manage chronic pain, improve mobility, or simply to stay fit and healthy, physical therapy services have proven integral in the current healthcare landscape, and they will continue to serve a critical role in the future.
Physical therapy (PT) is a crucial aspect of healthcare that serves to help patients heal from injuries, disabilities, and health conditions. Celebrated in October, National Physical Therapy Month aims to highlight the significant role PT plays in improving quality of life. This profession has not only gained recognition for its effectiveness but is also crucial in the Veterans Health Administration (VHA), the largest integrated healthcare network in the U.S.
Currently, the VHA includes 3650 Physical Therapists and Physical Therapist Assistants spread across 1,255 healthcare facilities nationwide, extending comprehensive services to the 9 million Veterans enrolled each year. Given the vast symptoms and conditions that PTs are trained to treat, a physical therapist’s role is of paramount importance.
Battle Creek VA Medical Center (BCVAMC), a part of the VHA, is expanding its clinics currently based in Battle Creek, Wyoming, and Lansing to include Muskegon and Benton Harbor. These facilities’ PTs cater to an exhaustive list of nearly 140 symptoms and conditions recognized by the American Physical Therapy Association (APTA).
Common issues that PTs evaluate and treat include Amputations, Arthritis, Back Pain, Carpal Tunnel Syndrome, Fractures, Joint Replacement, Knee Pain, Pelvic Floor Disorders, Sciatica, Spinal Cord Injury, Sports Injuries, and Stroke. Different treatments apply to different cases, with PTs providing individually tailored treatment plans to address these patients’ specific needs and goals.
Despite the generalized perception of PT as just an instructive exercise regime, it goes far beyond that. The primary aim of PT is to facilitate recovery and enhance overall functionality, provided the patients are willing to put in the necessary work.
With military service members subjecting their bodies to varying degrees of stress due to numerous military and humanitarian operations, PT generally becomes their bridge to a better state of physical functionality. However, that does require a certain amount of dedication from the patients’ side, as highlighted by Kaitlin Ezinga, a physical therapist under the BCVAMC.
Noting that the benefits reaped from PT are directly proportional to the amount of effort invested in it, Ezinga expressed her satisfaction in seeing major improvements in patients’ abilities and their return to activities they previously struggled with. Positive feedback from patients is not only rewarding, but it also enriches the overall therapeutic journey, instilling a sense of achievement in the therapists.
The BCVAMC currently has a team of 19 physical therapists, 6 physical therapy assistants, and has an expansion plan underway to cover 21 counties with focused provisions for Pain, Primary care PT, Amputee, Gerofit (exercise for older adults), Aquatics, and Pelvic/Women’s health.
PT has a profound effect on the quality of life, with inadequate physical activity leading to an additional $117 billion in health care costs in the U.S along with reduced quality of life for millions of Americans. However, the use of PT in treating various conditions such as osteoarthritis of the knee, carpal tunnel syndrome, and low back pain, among others, has proven to be beneficial and cost-effective.
Based on APTA’s net benefit analysis of PT services per episode of care for eight conditions, they concluded cost-saving ranging from $2,144 for falls prevention up to $39,533 for carpal tunnel syndrome. Considering these numbers, the perception of PT is shifting from an optional supportive practice to an essential component of healthcare, improving health outcomes, and reducing overall treatment costs.
Particularly in a context like the VHA, working with Veterans who often bear the physical tolls of their service, the positive impacts of physical therapy become even more apparent. Ezinga, relishing in the privilege of serving those who have served the country, epitomizes the mutual respect and appreciation that bind physical therapists and their patients in a rewarding therapeutic relationship.
Sources:
 Dr. Sean Wells, et al. v. Kennedy, et al.
Dr. Sean Wells, et al. v. Kennedy, et al. Physical Therapy Services Now Available at Sanford West Fargo
Physical Therapy Services Now Available at Sanford West Fargo- Vyana Expands Online Physiotherapy Services for Global Patients
- New physical therapy practice opens in Cranford
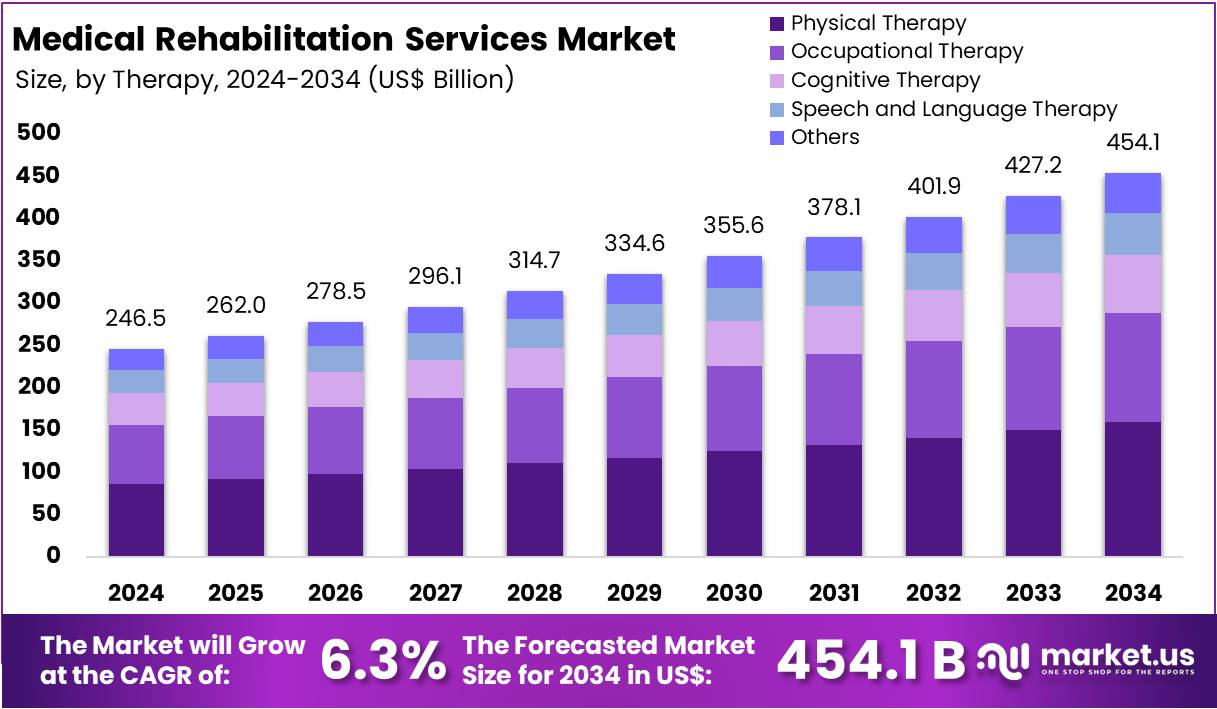 Medical Rehabilitation Services Market Size | CAGR Of 6.3%
Medical Rehabilitation Services Market Size | CAGR Of 6.3% KKU Physical Therapy Elevates Sports Services, Launches Sport PT Mobile Clinic
KKU Physical Therapy Elevates Sports Services, Launches Sport PT Mobile Clinic State of Direct Access to Physical Therapist Services: A Report from the American Physical Therapy Association
State of Direct Access to Physical Therapist Services: A Report from the American Physical Therapy Association National Physical Therapy Month: A Quality of Life Healthcare Service | VA Battle Creek health care | Veterans Affairs
National Physical Therapy Month: A Quality of Life Healthcare Service | VA Battle Creek health care | Veterans Affairs